Laminitis Fact Sheet
Laminitis is widely recognised as one of the most crippling diseases to horses and ponies; it is an extremely devastating and complex disease that shortens working lives with the potential for euthanasia. Traditionally considered a disease of fat ponies eating too much lush grass, it can actually affect any horse, of any age, or sex, at any time of the year, and although, predominantly a disease of the forefeet, it may affect one, or all four hooves and can be triggered by a variety of metabolic, or physical causes. Most horses, and ponies recover from laminitis, but their recovery is highly variable and dependant on many factors.
What is laminitis?
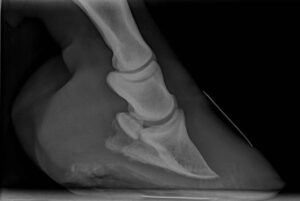
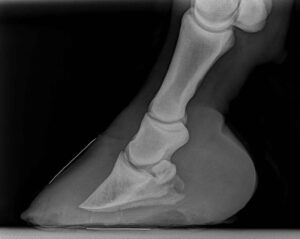
Laminitis is an extremely painful inflammatory condition of the laminae tissues of the hoof. The laminae are made up of two bands of strong slightly elastic tissues that are found on the pedal bone and the hoof wall. On the hoof wall, growing from the coronary band are the insensitive laminae (a bit like our fingernail) and on the pedal bone, the sensitive laminae (similar to the sensitive skin under the fingernail), which interlock with each other. The laminae carry the whole weight of the horse, so must be in perfect health and condition. When inflammation of the laminae occurs (laminitis), the laminae are weakened and can result in painful tearing of the pedal bone laminae from the hoof wall. As laminitis develops the attachment of the pedal bone to the hoof wall can start to fail allowing the pedal bone to either rotate within the hoof, or drop, which can be fatal.

Recognised Risk Factors Causing Laminitis
Although traditionally considered a disease of fat ponies over eating-eating lush green grass, laminitis can affect any horse, or pony, of any age, or sex and can be triggered by a variety of metabolic or physical causes. Laminitis is multi-factoral, therefore usually means that there is more than one factor involved before the animal succumbs to the disease.
Nutritional causes of laminitis
Excessive intake of:
- Lush grass; and the readily available sugars it contains directly available to the digestive tract.
- Similarly, poor pasture; with grass stressed due to overgrazing, or frost results in the formation of readily available sugars.
- Highly molassed feed; although most sugar is digested in the small intestine, excessive sugars in the diet may reach the hindgut
- Cereal grains; grains contain starch in the form of carbohydrates, which are broken down to simple sugars in the digestive tract.
All the above factors contribute to an overload of soluble carbohydrate and an excess of sugars into the hindgut, from the foregut causing a gastrointestinal disturbance; these changes somehow precipitate laminitis.
Increased levels of sugars entering the bloodstream from both the foregut and the hindgut can also somehow trigger diet induced laminitis, through temporarily raised insulin levels in the blood relative to the levels of glucose (hyperinsulinemia).
Therefore it is important to feed a low sugar, low starch, high fibre diet, with calorie intake controlled where necessary.

Non- nutritional causes of Laminitis:
These can be attributed to physical stress/ trauma on the body, underlying/ past medical problems, or metabolic factors initiating hormone changes, such as an overproduction of cortisol.
- Dependent laminitis; where severe lameness in one hoof causes excessive weight on opposing limbs
- Traumatic laminitis; repeated physical trauma to the hooves: hard ground, jumping, endurance riding, worked too soon etc.

- Incorrect/ late farriery; delays between foot trimming, or shoeing can cause stress or damage to the laminae. Regular farrier visits should also pick up early warning signs of laminitis.
- Toxaemia; bacteria release toxins during certain illnesses: retained placenta/afterbirth after foaling, colic, diarrhoea etc.
- History of laminitis; past sufferers are more susceptible to re-occurrence
- Stress; from long distance transport may also be considered a hormonal issue.
- Administration of certain medications; such as corticosteroids injected as an anti-inflammatory increase cortisol hormones in the body.
- High Insulin Levels; underlying health problems, such as Equine Metabolic Syndrome (EMS)
- Obesity; not only adds to the mechanical weight that the hooves directly support, but also has a negative effect due to the fatty pockets in the stomach releasing hormones such as cortisol. Obese horses are also more likely to be Insulin Resistant (IR), or suffer from EMS.
- Hormonal / Metabolic (Endocrine) Influences; Pituitary Pars Intermedia Disease, Equine metabolic Syndrome, Insulin Resistance, or other endocrine disorders can lead to laminitis as a secondary issue:
- Pituitary Pars Intermedia Disease (PPID), more commonly known as Equine Cushing’s Disease (ECD); is the most common endocrine disorder, typically occurring in horses over 15 years of age, caused by enlargement of the Pars Intermedia (middle section) of the pituitary gland located at the base of the brain. Dysfunction of the Pars Intermedia results in the release of several hormones, one of which ACTH, causes the adrenal glands to produce the stress hormone cortisol. Persistent levels of cortisol and other hormones can increase blood sugar (glucose) and supress the immune system.
- Equine Metabolic Syndrome (EMS); referred to as a peripheral Cushing Disease, primarily occurring in horses younger than 15 years, is both a metabolic and hormonal disorder characterised by obesity and insulin levels. Obese horses with excess fatty tissue can develop insulin dysregulation, having an increased insulin response to sugars causing a subsequent rise in blood insulin levels (hyperinsulinemia), which can result in insulin resistance.
- Insulin Resistance (IR); is a hormonal disorder that most commonly occurs in animals suffering with PPID, or EMS. Sugars from foods fuel metabolic processes and supply energy to the body. Insulin is produced by the liver in response to elevated blood sugar (glucose) levels by signalling fat, muscle and liver cells to take up glucose from the blood and store it as glycogen. Insulin will be produced after the animal has eaten a starchy, or high sugar meal. However, insulin resistance occurs when the cells become resistant to the sugar uptake action of insulin. The body then produces more insulin to counteract this and in the short term is successful. However, in the long term, the increased insulin cannot maintain optimum blood sugar levels; therefore the body then has elevated levels of both insulin and glucose circulating.
Clinical Signs of Laminitis
Sudden Onset Signs:
- Reluctance, or inability to walk
- Increased respiratory rate – panting and sweating
- Glazed, pained expression
- A stance with the hind feet under the body and forefeet camped out, or resting/ rocking back on the heels
- Bounding digital arterial pulses
- Feet hot to touch
- In cases where all four feet are affected the horse may stand with all feet tucked under the centre of their body, and in severe cases will be recumbent and unable to rise.
- In severe cases where the coffin bone has sunk, a depressed area is usually visible immediately above the coronary band; blood can sometimes ooze out of here.

Milder or Chronic Signs:
- Shifting weight from one limb to another
- Lifts alternate feet
- Reluctant to move, or stand on hard surfaces
- Pottering gait – whereby there might be a slight change in the animals gait, moving in a “pottering” fashion, or a stiffness to their walk
- Heat in the hooves
- Increased digital pulse
If you suspect laminitis, or have any concerns call your veterinarian immediately; the disease can be well under way for 40 hours prior to any clinical signs showing. Studies have shown that recovery is more likely when veterinary attention is received promptly.
Recent research suggests that 1 in every 200 horses will require veterinary attention each year due to laminitis.
While you are waiting for your veterinarian to arrive DO NOT:
- Feed
- Medicate
- Force to walk
- Place feed in cold water, or ice
However, if possible, if your horse will walk, lead your hose to a heavily bedded stable with shaving; make sure you do not use a straw bed as your horse may eat it.
Diagnosis
In most cases the diagnosis of laminitis is obvious, but in all cases a vet should be consulted to confirm the diagnosis, determine its severity and possible underlying cause and devise an appropriate treatment method. This will usually require taking a complete history, a full examination, blood tests and radiographs (x-rays).
Treatment
It is absolutely essential that you contact your vet should your animal show any signs of laminitis. The treatment of this disease can be time consuming and costly, and involves a lot of commitment from the horse owner; you have to be prepared to change your animals management for the foreseeable future, perhaps even for the rest of their lives.
- Farriery – is a vital part of laminitis treatment and ongoing management. The farrier may decide to remove a small portion of the hoof wall & with veterinary involvement may remove the entire front wall of the hoof, usually know as dorsal wall re-section.
- Hoof Care Padding/ Frog Supports – available from the vet or farrier. These are used to support the frog/ coffin bone to relieve pressure on the laminae. Heels may also be elevated to reduce the pull of the deep digital flexor tendon.
- Non-steroidal anti-inflammatory drugs (NSAIDs) – such as phenylbutazone (Bute), flunixin meglumine (Banamine), or acerpromazine (ACP). If pain relief is required other drugs can be given, although caution is warranted, as a horse that can’t feel foot pain may become too active, further damaging the feet.
Box rest – Strict box rest should be adhered to, as the animals chance of a full recovery are reduced and the recovery period longer if box rest is ignored. The stable should be well bedded down, ideally with 18” of clean dry wood shavings over the entire floor area. Standard advice is 30 days box rest; however this may vary depending on the animal’s condition. It is advisable to keep the animal in box rest until they move freely and are off all drugs. Nonetheless, once the hoof capsule is stable exercise is beneficial, especially for those diagnosed with EMS/ IR, as exercise reduces blood insulin levels.
- Where the trigger for laminitis has been attributed to nutritional factors it is important to manage the animals’ diet, specific to each individual horse. Standard advice suggests cutting out any cereal based compound feed, limit forage and instead feed a high fibre, low sugar and low starch diet of chopped feeds with plenty of fluids; usually based on 1% of body weight per day with a balancer. It is important to reduce sugar and starch intake to a minimum in case an insulin response is involved and to re-establish the correct bacterial population in the hindgut, whereby the fibre digesting bacteria dominate and the bacteria which digest sugars and starch are not allowed to proliferate excessively. Honeychop Chopped Oat Straw is the ideal fibre feed with a combined sugar and starch level of only 2.2%.
- NEVER starve a laminitic this can cause hyperlipaemia and be fatal.



Prognosis
Most horses, and ponies recover from laminitis, but the prognosis of their recovery is highly variable and dependant on how quickly it was spotted, the number of hooves affected, the time it was left untreated and how advanced and severe the case of laminitis has become. Other factors contributing to recovery include the underlying cause, pre-existing medical conditions, if the equine has previously suffered from the disease and ultimately response to treatment. In severe cases, if the equines pain cannot be controlled then they may have to be euthanised. Even, if there is a chance that the equine may recover over time, euthanasia may have to be considered instead of letting them suffer over weeks or months of treatment, until the pain resolves. A recent study showed 1 in 5 horses and ponies with laminitis were euthanised.
Tips for Prevention
While not all cases of laminitis can be prevented, you can help reduce the chances by the following:
Weight control
- Maintain appropriate body condition – Measure and record your animals’ weight using a weigh tape, or bridge every two weeks and condition score.
- As a rule of thumb at ideal weight you should be able to feel your animals’ ribs but not see them and they should not be carrying a fat crest, or fat pads over the loins, or tail head.
- It helps to ensure that your horse or pony is in the correct body condition before you turn out in the spring, as you cannot diet a horse on grass.
- Exercise in overweight animals is the most effective way to control bodyweight.
- Up to 50% of the horse population in the UK are overweight, yet on average only around 25% of horse owners recognise their animal need to lose weight.

Feeding Guidelines:
- Manage grazing – Restrict intake of lush grass via a grazing muzzle. Do not turn animals out onto frost, or stressed paddocks. Consider strip grazing, or mixed grazing with sheep. Optimal grazing times are early morning and late nights when the fructans (sugars) are at their lowest.
- Minimise, or eliminate concentrates (grains and cereals) from the diet.
- Feed a high fibre diet, with less than 10-12% non-structural carbohydrates (NSC) for example Honeychop Chopped Oat Straw, but ensuring that adequate water is consumed to avoid the risk of colic, or gastric ulcers; this can be in the form of hay, or a chopped hay replacer.

- Soaking hay from two to twelve hours will assist water intake and also leach out some of the protein, carbohydrates and sugars; soaked fibre needs to be rinsed well and fed immediately. All fibre needs to be weighed and triple netted with small holed hay nets, or specifically designed slow feeding hay nets.
- Using a hay replacer, such as Honeychop Chopped Oat Straw may prove to be a useful alternative instead or having hay analysed and trying to find hay with less than 10% NSC it also eliminate the requirement to soak hay in winter months. Honeychop Chopped Oat Straw is a Free From product and contains no oil, or molasses, and gives it an NSC of only 2.2%.
- Avoid bran. Due to its high phosphorus content feeding it over a log period will result in low levels of calcium; another vitamin important for hoof health.
- Use quality vitamin and mineral supplements, or feed with supplements already in.
- Changes to diet need to be gradual.
- Feed little and often and always make sure your equine has access to clean fresh water (be extra vigilant in winter months as water may freeze over)
Hoof Health
- Regular professional foot care – regular trimming and correct foot balance are essential for healthy feet. Specialist shoeing can assist – speak to you farrier to discuss whether this is appropriate.

General Health
- Monitor your horse following medical conditions such as colic or retained placenta – these are high risk causes of laminitis
- Test for Cushing’s Dieses (PPID ), Equine Metabolic Syndrome (EMS) and Insulin Resistant (IR) A very high number of horses and ponies suffer from insulin resistance due to EMS and PPID. IR can be tested for by a blood glucose assessment and there is an accurate blood test for PPID and EMS.
Work
- Avoid excess work on hard surfaces, as concussion can cause laminitis.
- Avoid any form of stress. Stress may predispose your equine to develop laminitis. When stressed, equines release corticosteroids from their adrenal gland. Alterations in blood flow to the feet may then promote laminitis.
- Feed according to size, work load and climate.
Once your horse or pony has had laminitis, they are more predisposed to future episodes; make sure you manage them appropriately to avoid future problems.